Manoj Pandey*
I have taken the liberty to generalize some concepts for the sake of simplicity. Puritans may please forgive me for that.
As we often do in this column, let me brush up your knowledge on this basic subject, which you might have forgotten after you studied it in your school.
At the core of all life, there is some form of genetic material. To become ‘genetic’, the chemical must be able to store all the information about its biological self in a way and form that it can be used for carrying out all life-activities and also be passed on to the progeny. It is said that life originated and evolved on the earth after such a chemical developed due to special conditions that existed billions of years ago. The chemical is called nucleic acid.
If you magnify a molecule of the genetic material (nucleic acid) millions of times, you see it in the form of a string in which certain molecular segments repeat in a specific sequence.
These segments are called nucleotides. Each nucleotide has a sugar molecule attached to a phosphate ion. To the sugar, a nitrogenous base is attached. The nucleotides together make the string, like a chain is made out of links. Based on the type of sugar, these strings of genetic material are called DNA (deoxy-ribo nucleic acid) or RNA (ribo neucleic acid).
The full set of DNA and/or RNA in a living cell is called its genome.
There are 4 types of nucleotides and their arrangement in the string of DNA or RNA determines the information that the strand carries.
In most living beings, except some viruses, DNA is the main genetic material though RNA is still required for many cellular functions. In some viruses, including coronaviruses, RNA is the only genetic material.
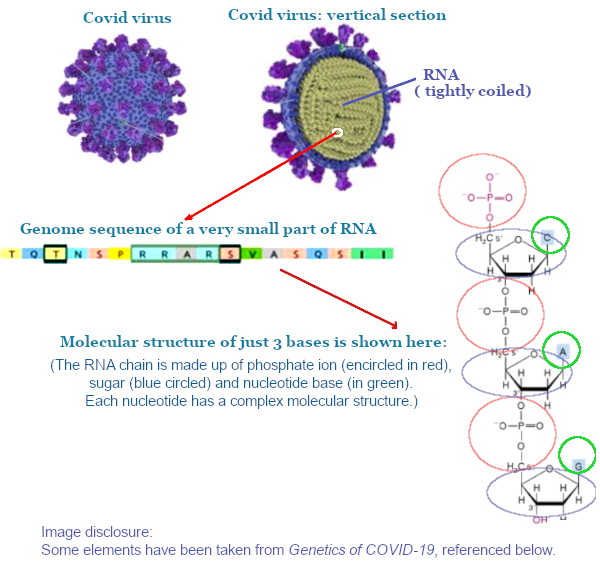
COVID-19 virus’s genome consists of a single thread of RNA with nearly 30 thousand nucleotides (and some supplementary chemical constituents, and a structural protein to keep the RNA in shape).
When COVID-19 virus enters a human cell, its RNA gets activated at 50 locations and subjugates the host cell to start creating that many types of proteins by translating the information contained in different segments of the RNA. The symptoms are caused by these proteins or the body’s reaction to them. The virus RNA uses some of the proteins created by it and many host resources to replicate itself in large numbers and infect other cells.
Let us recap these basics by defining the terms used as these will be used in the rest of the article:
- Genome= The full genetic makeup of a living being, in the form of DNA and/or RNA.
- RNA or DNA= The long chain of molecular units (phosphate + sugar + nitrogenous base) called nucleotides, that acts as genetic material. All the RNA or DNA strands together make up the genome. The particular sequence of these nucleotides is what stores information for producing genes as well as transferring traits from the parent to the progeny.
- Gene= A functional unit of the RNA or DNA that carries out a specific function, e.g. producing a particular protein. A gene consists of many, sometimes thousands, of nucleotides.
Now the main subject.
- What are mutations?
DNA and RNA need to replicate so that they pass on their information (which is coded in the form of specific sequences of nucleotide bases) to the progeny or for various life-processes.
The process of replication, however, is not fail-proof, and the sequence of nucleotide bases in the resulting threads is sometimes not copied correctly from the parent thread. That is called mutation.
If the creature has very small genetic material, it breeds fast and in large numbers, there are chances that its genome soon has many mutations that are significant. Thus, viruses – because they produce trillions of new viruses over billions of replications every few hours, in a pandemic situation – can have numerous mutation within a few weeks or months.
You can imagine the extent of mutations in the coronavirus from the fact that even with limited genetic sequencing facilities, the Indian National Task Force stated in February 2021 that Indian labs had detected more than 7000 variants with over 24000 mutations among Indian patients.
- Are mutants different from variants and strains?
When a virus mutates in a way that we can pin-point the mutation, we call it a ‘mutant’. The COVID-19 virus (SARS-CoV-2) must be having lakhs of mutants, and scientists have documented many thousands of them.
When the mutation is well-defined in molecular terms and is of some significance in terms of virulence, we call the mutant a new ‘variant’. A variant usually has many mutations, so its pathogenic properties are distinguishable from other variants.
When the mutation is big and changes the working of the mutant virus in a significant way as compared to the parent virus, we call it a new ‘strain’.
The terms variant and strain are sometimes used interchangeably, especially for new mutants, before scientists are able to say definitively how significant the mutation is.
From the point of view of health monitoring, the new variants or strains are categorised according to how harmful they are: Variant of Interest (VOI), Variant of Concern (VOC), or Variant of High Consequence (VOHC).
Some well-documented variants are the UK variant, California variant, Brazil variant, South African variant, Indian double mutant and Indian triple mutant. These are not scientific names and the present naming system (in which the UK variant is called B.1.1.7) is also not universally accepted as it is far from being perfect.
- Are mutations making COVID-19 virus more severe and fast-spreading?
Mutations are ‘value-neutral’: they are errors in the replication of the genetic strand.
Mutations can work against or in favour of the virus.
Mutations can also work at cross purposes to one another. So, we will soon have variants with thousands of combinations arising out of very high to very low virulence and very high to a very low speed of spread.
Another natural process that works together with mutations is natural selection or how nature favours or disfavours the variant. Thus, the mutations that lead to fast spread are likely to help the virus spread much wider as compared to others. Similarly, if a mutant becomes highly lethal, it will not be able to spread far and wide because the infected people will die before they spread the virus to a large number of people. (However, when the disease has reached a pandemic stage, this disadvantage will be compensated by the sheer number of infections, and overall deaths might keep rising).
When a human population is infected by a number of variants with different characteristics, they increase the likelihood of infection because every individual might not have the strength to ward off all variants.
In the Indian population, in March 2021, all the major variants found in the world as well as some that originated in India were in circulation. That is one of the reasons for widespread infections in ‘the second wave’ of COVID-19 pandemic in India. However, as the infection becomes widespread, the competition among variants to find a vulnerable person will lead to a situation in which only one or two variants will remain in the battlefield.
- Do viruses that originate in one place remain in that place?
No. The WHO informed in January 2021 that the virus that was first observed in the UK (the UK variant) had been found in 70 countries and the South African variant in 31, and the spread is ongoing. Even the newly-detected Indian variants have reached nearly two dozen countries by April 2021.
Restriction on movement from other countries or regions, and quarantine, are likely to contain different variants within certain geographies or check their spread in new geographies, but in the case of a pandemic of COVID-19 scale, that might not work too well. It has been reported that almost all the major known variants have been detected in the American population, despite strict travel checks.
- Does a double mutation mean it is double in potency?
Double mutations and triple mutations do not directly convey that the mutated virus is virulent or infectious those many times. It just shows that the variant shows mutation at two or three sites in its RNA strand.
Other things being equal, a triple mutant might be different from the original virus in more ways than a single mutant. But that may or may not favour the virus.
- Do vaccines and a high level of infection reduce mutation?
It is clear from the above discussion that if the virus spreads less, it will replicate less, and the chances of its mutation will be lower. So, if a population is well vaccinated, follows COVID-appropriate behaviour and is already infected to a big extent, replication of the virus will slow down to that extent, leading to fewer variants emerging too soon.
Conversely, in a large population in which the virus has been infecting people in significant numbers over a long period, hundreds of mutations would occur, some of them would lead to the creation of new variants, and a few might turn out to be variants of concern.
- A person has escaped infection so far. Is he more likely to be infected by new variants?
Since mutations lead to a change in behaviour of the virus (e.g. its mechanism for attaching to human cells), new variants often cause different symptoms in the infected people, and their virulence, mechanism of spread, etc can be different from its parent variant. So, pathologically, a new variant may be able to attack a person who has not been infected by other variants.
All the commonly-known variants are Variants of Concern because they are known to be either more infectious or more virulent. This is the reason, national authorities must try to check the spread of these variants in the population by testing and tracking people entering the country.
- Can a new variant infect one who has developed antibodies against a previous variant?
Antibodies work in a complex way in defending the body against attack by a pathogen. They remember the earlier attack, and they also have a specific way of neutralizing the attacking pathogen. In normal conditions and in the early stages of a disease/ pandemic, new variants are not so different from the earlier variant and, therefore, antibodies are able to guard the body against new variants. If the new variant is too different from the earlier ones, the antibodies will not be able to identify the pathogen (virus) as an enemy or will not be able to neutralize it. In the case of COVID-19, such a stage has probably not arrived yet, but is likely to arise in the coming years.
The response of antibodies against pathogens of similar type is not a categorical ‘friend’ or ‘foe’; it may differ in degrees. Therefore, it is likely that the antibodies developed against an earlier variant are not fully potent against a new variant but are able to protect the body to at least some extent.
- Are the existing vaccines not effective against new variants?
The above answer would relate to vaccines also. Vaccines simulate a viral attack and induce the human body to produce antibodies.
The actual efficacy of a vaccine against particular variants depends also on the type of vaccine and against how many variants it was tested during the development stage and checked after release.
As of now, there is not enough data to show if a vaccine is less effective against a particular variant. Vaccine producers are claiming that their vaccines are potent against all known variants of concern.
As said above, the response of antibodies against an infection may be graded. As such, even if a vaccine is not fully potent against a new virus, it is likely that the infection by a new variant will be less severe among vaccinated people.
- Are the present tests not good for new variants?
Since new variants can attack a different area of the respiratory tract or may have different symptoms or can lead to different types of reactions from the human body, the existing tests for infection may become less precise for new variants. For example, the Indian variants are reported to be attacking the lungs directly while the original variant used to colonize the nasal tract before attacking the lungs. So, while nasal swabs could capture the earlier variant even at the initial stage of infection, the new variant virus is difficult to be captured by tests using swabs collected from the nose or throat.
- Is that the earlier treatments are proving less effective against new variants?
Perhaps. For example, there are media reports that in the US, patients infected by the UK variant or the South African variant were not responding to the earlier treatment regimen. This happens when the new variant uses a different mechanism for attack or produces a different type of reaction from the human body.
- Will we need to take a jab every now and then due to virus mutations?
The COVID-19 coronavirus is not mutating as much as some other coronaviruses, e.g. the one causing viral flu. But if some mutations help the virus escape antibodies developed by the existing vaccines or some big mutations lead to the creation of new strains of this virus, re-vaccination will be required. In the case of the common flu virus, it has distinct strains endemic to different areas, and the virus also mutates rather fast. Therefore, a new jab is required after a gap and when one travels to a region where a different viral strain is prevalent.
In addition, there has not been much research on how long the antibodies remain effective against the COVID-19 virus. It is apprehended that antibodies caused due to infection or vaccination might not last more than a few months. If so, repeated vaccination will be inescapable whether the virus mutates in a big way or not.
- Is large-scale vaccination one reason for the virus adapting itself by causing new variants of itself?
As discussed earlier, mutations are not directed or deliberate; they are random errors. So, the virus cannot use mutations for adapting itself to anything that humans do to protect themselves.
Some mutations can give the virus the ability to escape the immunity induced due to earlier infections or vaccination. Such variants will be favoured by nature and become more prevalent. This is the way organisms evolve.
On the other hand, more vaccination reduces infection in the population, thus a large number of viruses perish without giving rise to new progeny. The breaking of the chain, thus, can lead to the formation of a lesser number of variants.
- Are new variants likely to infect children more?
That cannot be ruled out. It needs just a few mutations that help the virus exploit vulnerabilities in children. For example, children’s bodies are less exposed to diseases and their diaphragm may not be not strong enough to bear much strain.
Further reading

*About the author: This article has been contributed by Manoj Pandey. He does not like to call himself a rationalist but insists on scrutiny of apparent myths as well as what are supposed to be immutable scientific facts. Please don’t take the views of the author as the views of Raag Delhi.



